For ABA providers, ABA authorization management has become a critical operational responsibility. Clinics must track approved therapy hours, monitor authorization periods, and ensure services stay within payer coverage limits. When authorizations are not managed properly, providers risk denied claims, administrative delays, and interruptions in care.
At the same time, regulatory oversight around ABA billing and documentation continues to grow. In March 2026, the U.S. Department of Health and Human Services Office of Inspector General released a report examining Medicaid payments for ABA services in Colorado. Auditors found $77.8 million in improper payments and $207 million in potentially improper payments, largely tied to documentation and compliance issues rather than fraud.
The report highlights an important reality for ABA organizations: strong operational systems are essential. Authorization tracking, documentation, scheduling, and billing must work together to ensure services remain compliant with payer requirements.
Understanding ABA Authorizations
Before ABA therapy services begin, most insurance payers require prior authorization. This approval confirms that the payer agrees to cover services under specific conditions.
Authorizations usually include several important elements:
- Approved procedure codes
- Authorized units or therapy hours
- Authorization start and end dates
- Payer-specific billing rules
These parameters define the limits of coverage. If services are delivered outside those limits, claims may be denied.
Because of this, authorizations affect multiple areas of clinic operations. They influence scheduling decisions, treatment planning, and billing eligibility. When authorization data is inaccurate or difficult to track, operational issues can quickly arise.
Why Managing Authorizations Is Challenging for ABA Clinics
Authorization management becomes more complex as clinics grow.
Each client may have multiple authorizations throughout the year. Different payers have different requirements. Treatment plans evolve as therapy progresses.
Many ABA practices still rely on manual tools such as spreadsheets to track this information. While spreadsheets may work for smaller caseloads, they become difficult to maintain as organizations scale.
Common challenges include:
- Tracking dozens or hundreds of active authorizations
- Monitoring remaining therapy hours for each client
- Keeping track of authorization expiration dates
- Coordinating information across scheduling and billing systems
When these processes are not centralized, mistakes become more likely. A missed expiration date or incorrect unit count can quickly lead to denied claims.
Compliance Risks and Improper Payments
Recent federal audits demonstrate why authorization oversight matters.
The OIG report reviewing Colorado Medicaid ABA claims found that nearly every sampled claim included at least one documentation or billing issue. Many improper payments were related to missing documentation, incomplete service descriptions, or services delivered by providers without the appropriate credentials.
Other potential issues identified in the report included:
- Services billed without clear descriptions of the therapy provided
- Activities that may not qualify as reimbursable therapy
- Charges for non-therapy time
- Group services potentially billed as individual therapy
The report does not suggest that these issues reflect fraud or poor clinical care. Instead, it highlights how easily operational gaps can lead to billing errors or compliance concerns.
For ABA providers, these findings reinforce the importance of maintaining strong operational systems that support documentation accuracy and authorization compliance.
Tracking Authorization Utilization
One of the most important aspects of authorization management is monitoring how many authorized units remain available.
Without clear visibility into utilization, clinics may discover authorization issues only after claims are submitted. By that point, services may already exceed the approved limits.
This problem often occurs when authorization tracking is disconnected from scheduling systems. Administrative staff may track units manually while scheduling teams assign therapy hours independently.
A better approach is real-time authorization tracking. When scheduling systems automatically update authorization utilization, clinics gain immediate insight into remaining therapy hours.
This visibility helps organizations:
- Prevent exceeding approved authorization limits
- Identify underutilized therapy hours
- Prepare reauthorization requests earlier
- Reduce billing errors
Avoiding Authorization Expirations
Authorization periods are just as important as authorized units. Each authorization has a defined start and end date. When the authorization expires, services must stop until a new approval is obtained.
Busy clinics may overlook expiration dates if they are tracked manually. This can create service disruptions and billing complications.
To avoid these issues, many providers implement proactive monitoring strategies such as:
- Reviewing upcoming authorization expiration dates regularly
- Preparing updated clinical documentation for reauthorization requests
- Submitting renewal requests before the current authorization ends
Automated alerts and centralized tracking systems can make these tasks much easier for administrative teams.
ABA Matrix Authorization Management
Managing authorizations manually becomes difficult as practices grow. Tracking approval periods, remaining units, and payer requirements across spreadsheets or disconnected systems can quickly create administrative complexity.
ABA Matrix simplifies authorization management by connecting prior authorizations directly to scheduling, service delivery, and billing workflows.
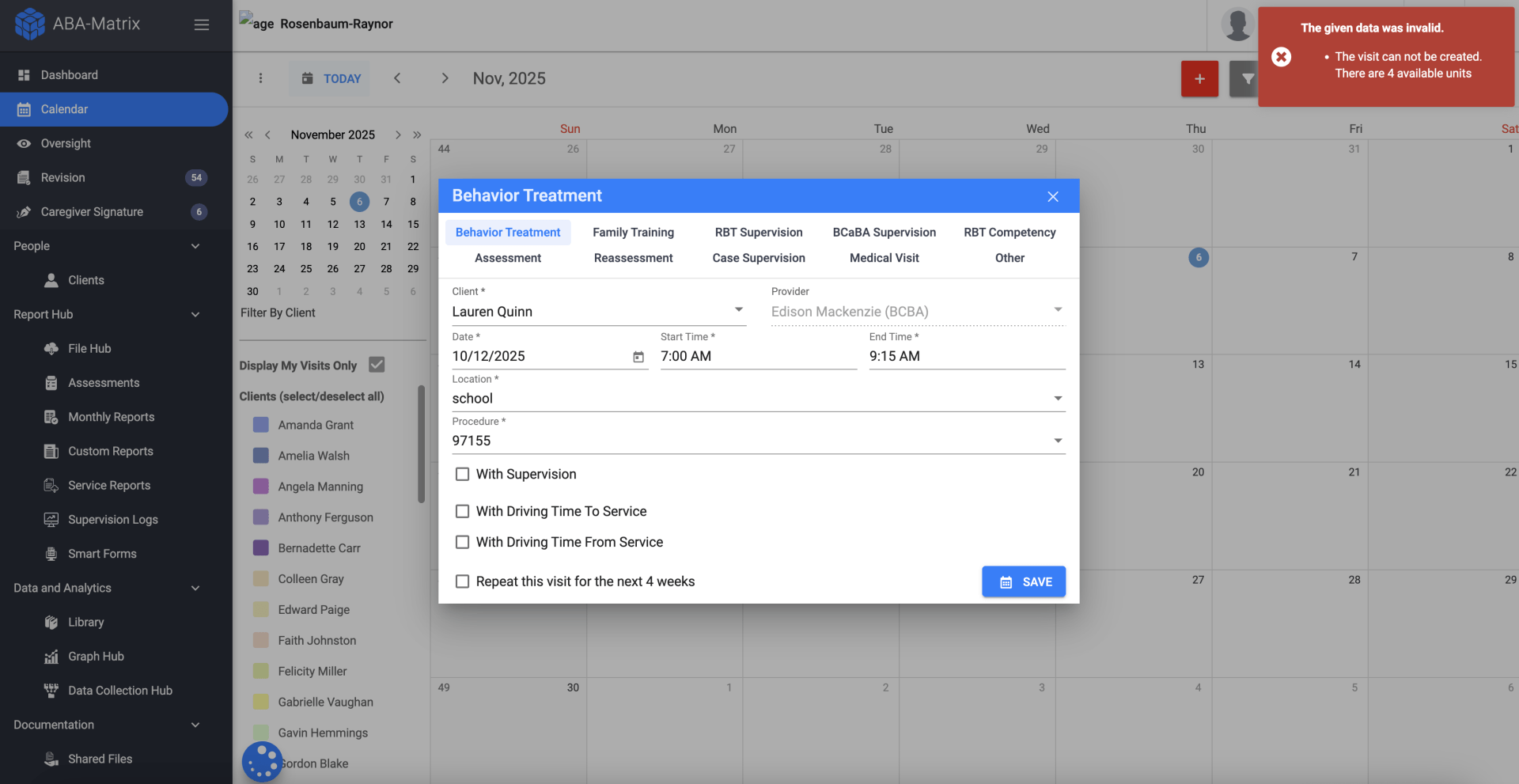
Authorizations can be added to the client profile with approved units and coverage periods, allowing teams to monitor utilization in real time as sessions are scheduled or updated.
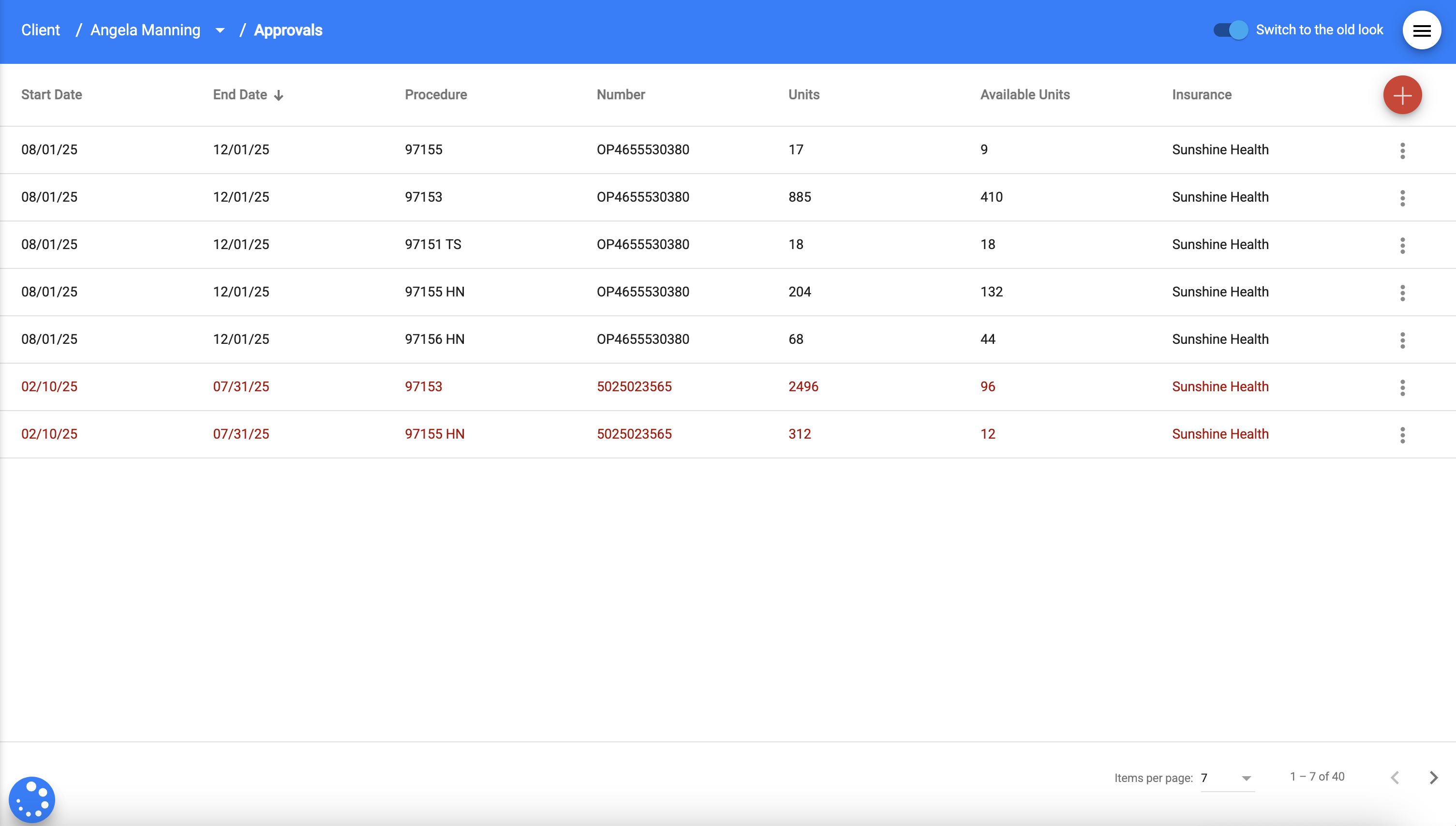
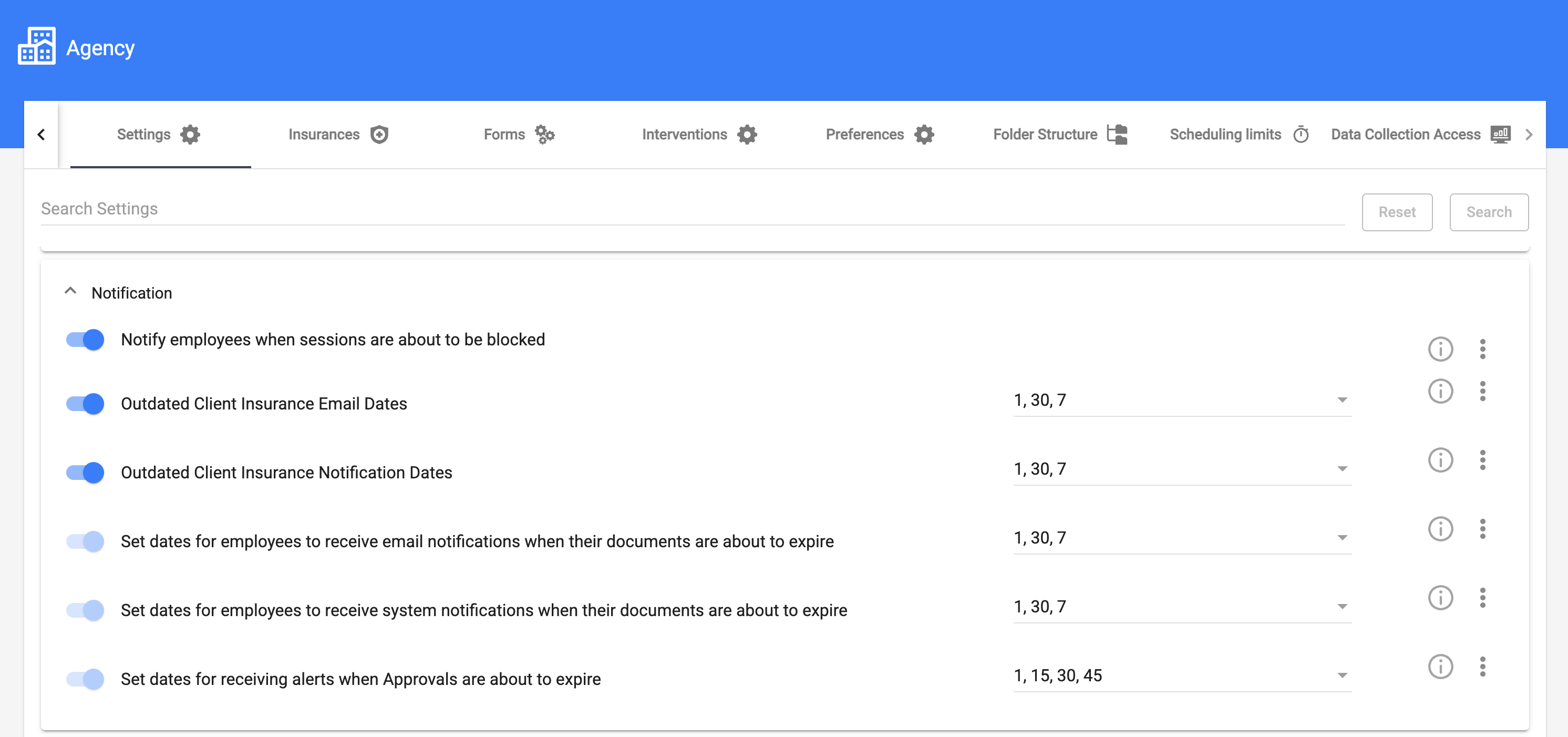
The system also provides alerts when authorizations are approaching expiration, helping clinics prepare reauthorization requests before services are interrupted. Built-in payer validation ensures that only covered procedure codes and modifiers are configured, reducing billing errors and supporting compliance with payer requirements.
Effective authorization management is essential for both operational efficiency and compliance in ABA organizations. ClABA authorization management
inics must track approved therapy hours carefully, monitor authorization periods, and ensure services remain within payer coverage limits.
As oversight around ABA services continues to increase, providers need reliable systems that support accurate documentation and billing workflows. Strong ABA authorization management practices help protect revenue, reduce administrative burden, and maintain uninterrupted care for clients.
When authorization tracking is integrated with scheduling, documentation, and billing systems, clinics gain the visibility they need to operate with confidence while focusing on delivering high-quality therapy.
