
A strong revenue cycle management (RCM) process is what keeps ABA therapy practices financially stable. But in ABA, revenue cycle management is not just about billing. It’s about making sure clinical care, documentation, and payer requirements all align so services can actually turn into revenue.
That’s where many practices run into trouble. Because in ABA, getting paid is not just about what you bill. It’s about what you can prove.
What Revenue Cycle Management Means in ABA Therapy
Revenue cycle management, a market projected to exceed $238 billion by 2030 according to a report from Research and Markets, refers to the process of managing how a healthcare organization gets paid for its services, from the first patient interaction all the way to final reimbursement.
In simpler terms, it’s everything that happens between scheduling a client and receiving payment for that service.
Revenue cycle management in ABA therapy includes verifying insurance coverage, obtaining prior authorizations, delivering services, documenting care, submitting claims, and following up on payments or denials. Each of these steps plays a direct role in whether a service is reimbursed.
Why Revenue Cycle Management in ABA Is Different
Revenue cycle management in ABA therapy works differently than in most areas of healthcare.
Every service must be justified before it happens, not after. It needs to be medically necessary, authorized in advance, and supported by measurable clinical outcomes. Even then, it must continue to demonstrate progress over time.
This level of oversight is driven in part by Medicaid requirements like Early and Periodic Screening, Diagnostic and Treatment (EPSDT), which require services to actively improve or maintain a patient’s condition.
In practice, this means revenue cycle management in ABA depends heavily on clinical accuracy. If the documentation doesn’t support the service, the revenue cycle breaks.
Understanding Revenue Cycle Management in Healthcare and ABA
At its core, revenue cycle management in healthcare refers to the full process of managing patient revenue, from intake to final payment.
In ABA therapy, that process includes several tightly connected steps: verifying insurance, obtaining authorization, delivering services, documenting care, submitting claims, and managing payments.
What makes revenue cycle management in ABA unique is how dependent each step is on the one before it. A small issue early in the process can create delays or denials weeks later.
It’s not a linear workflow. It’s a system where everything must align.
How the Revenue Cycle Works from Intake to Payment
Revenue cycle management in ABA starts well before the first session.
At intake, verifying insurance is about more than confirming active coverage. It involves understanding how ABA benefits are structured, whether a behavioral health carve-out is involved, and what authorization requirements apply. Industry benchmarks suggest this step should be accurate at least 98% of the time to avoid preventable denials.
Once eligibility is confirmed, prior authorization becomes the central control point in the revenue cycle. Payers typically require a complete clinical picture, including diagnosis, standardized assessments, and a treatment plan with measurable goals and caregiver involvement.
After authorization is approved, services must match exactly what was authorized. This includes the number of units, type of service, and provider credentials.
Before services begin, this process typically includes a clinical assessment and the development of a treatment plan, which are required to support authorization and guide care.
During service delivery, documentation becomes one of the most critical components of revenue cycle management. Notes must clearly reflect what occurred during the session, how it connects to the treatment plan, and what progress is being made. Start and stop times, objective data, and caregiver participation are all essential.
Only after all of this is in place does billing begin. Claims are submitted using standard formats such as CMS-1500 or 837P , and payment depends on whether every previous step holds up under payer review.
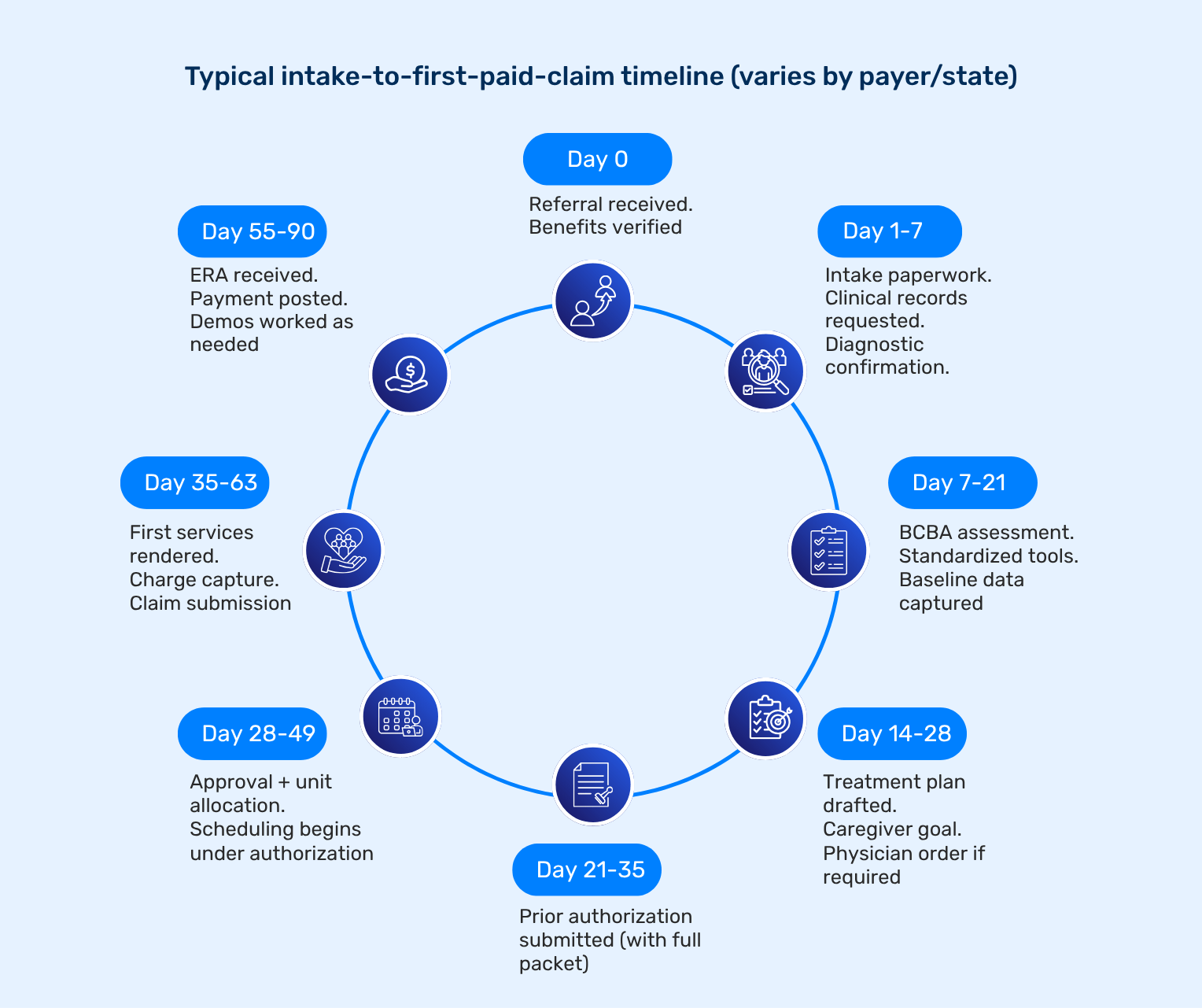
Revenue Cycle Management vs Medical Billing in ABA
It’s common to associate revenue cycle management with medical billing. But billing is only one part of the process.
RCM in medical billing focuses on claim creation, submission, and payment. But in ABA, most financial issues originate earlier.
A claim may be denied because the authorization does not match the service delivered. Documentation may not support medical necessity. Units may exceed approved limits, or modifiers may not reflect provider credentials.
By the time billing is involved, the issue has already happened.
That’s why strong revenue cycle management in ABA requires control across the entire workflow, not just the back end.
Where RCM Breaks Down in ABA Practices
When revenue cycle management is not fully aligned, certain patterns tend to appear.
Authorization issues are one of the most common. Units may expire, approvals may not match scheduled services, or requests may be incomplete. Documentation gaps are another major factor, especially when notes lack objective data or clear linkage to treatment goals.
Eligibility errors at intake can lead to claims being sent to the wrong payer, while coding or modifier inconsistencies can trigger rework even when services were delivered correctly.
Across healthcare, denial rates typically range between 5% and 10%, with top-performing organizations keeping them below 5%. In ABA, many of these denials are preventable because they originate in earlier stages of the revenue cycle.
How to Improve RCM Without Adding Complexity
Improving RCM in ABA does not require adding more steps. It requires strengthening the right ones.
High-performing organizations focus on accuracy at the front end. They ensure eligibility is verified thoroughly and consistently. They track authorizations in real time so services never exceed approved limits. They standardize documentation so every session note supports medical necessity and billing requirements.
Speed also plays a role. Reducing the time between service delivery and claim submission, ideally to just a few days, helps maintain steady cash flow and reduces exposure to filing limits.
These improvements are not complicated individually. The challenge is maintaining them consistently across the organization.
The Role of Healthcare Revenue Cycle Management Software in ABA
As ABA practices grow, managing revenue cycle management manually becomes increasingly difficult.
Disconnected systems create gaps between scheduling, documentation, and billing. Those gaps often lead to errors, delays, and lost revenue.
Healthcare revenue cycle management software is designed to reduce that friction. But in ABA, it must go beyond billing. It needs to connect the full workflow so that information flows seamlessly from one stage to the next.
Without that integration, teams are forced to rely on manual processes that increase risk.
How ABA Matrix Simplifies Revenue Cycle Management
ABA Matrix was designed to support revenue cycle management as a fully connected process, not a set of separate tasks.
- Scheduling is directly tied to authorizations, so sessions stay within approved limits.
- Documentation is structured to meet payer requirements and flows naturally into billing.
- Claims reflect exactly what was delivered, reducing discrepancies and rework.
This level of integration helps prevent errors before they reach the billing stage, which is where most revenue cycle management issues become visible.
Instead of adding more oversight, ABA Matrix builds accuracy into the workflow itself.
Why This Matters for ABA Practices
RCM in ABA therapy is not just a financial function. It’s an operational and clinical one.
Every step, from intake to documentation, influences whether services are reimbursed. When those steps are disconnected, small issues quickly turn into larger financial problems. When they are aligned, the entire system becomes more predictable and efficient.
That’s what allows practices to focus less on fixing errors and more on delivering care.
